Inhaltsverzeichnis
What is a Root Canal Treatment?
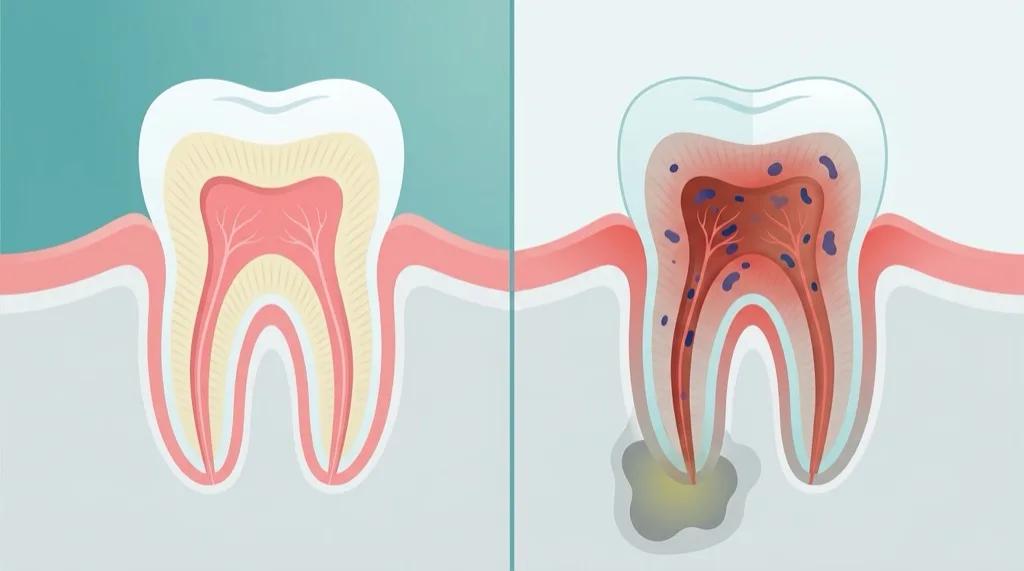
A root canal treatment — medically termed Wurzelkanalbehandlung (root canal therapy) or endodontics — is a tooth-preserving procedure that removes inflamed or dead dental pulp (the so-called pulp) from inside a tooth. The pulp is the living tissue within the tooth: a complex network of blood vessels, nerve fibres and connective tissue that extends from the coronal pulp chamber through the fine root canals all the way to the root apex.
When bacteria — usually through deep decay, a dental injury or cracks in the tooth — reach the pulp, inflammation develops (pulpitis). In advanced stages the pulp cells die (pulp necrosis) and bacteria spread through the root canals to the surrounding bone and soft tissue. The result is a periapical lesion — a focus of infection at the root tip that appears as a dark shadow on X-ray and can cause significant pain and swelling.
Root canal treatment solves this problem by completely removing the inflamed or necrotic pulp, thoroughly cleaning and disinfecting the canals, and then permanently sealing them with a biocompatible material. The tooth remains in the jawbone — it simply loses its vitality, but can continue to perform normal chewing function.
The poor reputation of root canal treatment comes from a bygone era without local anaesthesia and without modern magnification technology. With contemporary anaesthesia and microscopic precision, treatment today is largely pain-free — and significantly more effective than in the past.
Why Saving the Tooth Always Comes First
The most important principle of modern dentistry is: preserve the natural tooth before considering replacement. Your own treated tooth is biologically, functionally and economically superior to the alternative — extraction followed by an implant — in almost every case.
The jawbone around the tooth is maintained through natural chewing forces. An implant can also preserve bone, but first requires extraction, a healing period of three to six months and a surgical procedure. The total cost of an implant — including abutment and crown — typically ranges between €2,000 and €4,000, whereas the patient co-payment for modern root canal treatment is generally between €150 and €600. Investing in tooth preservation pays off on multiple levels — biologically, functionally and financially.
Symptoms — When Is Root Canal Treatment Necessary?
Not every toothache immediately requires root canal treatment — but certain types of pain and clinical signs are clear warning signals. The earlier endodontic treatment is initiated, the higher the success rate and the less extensive the procedure needed.
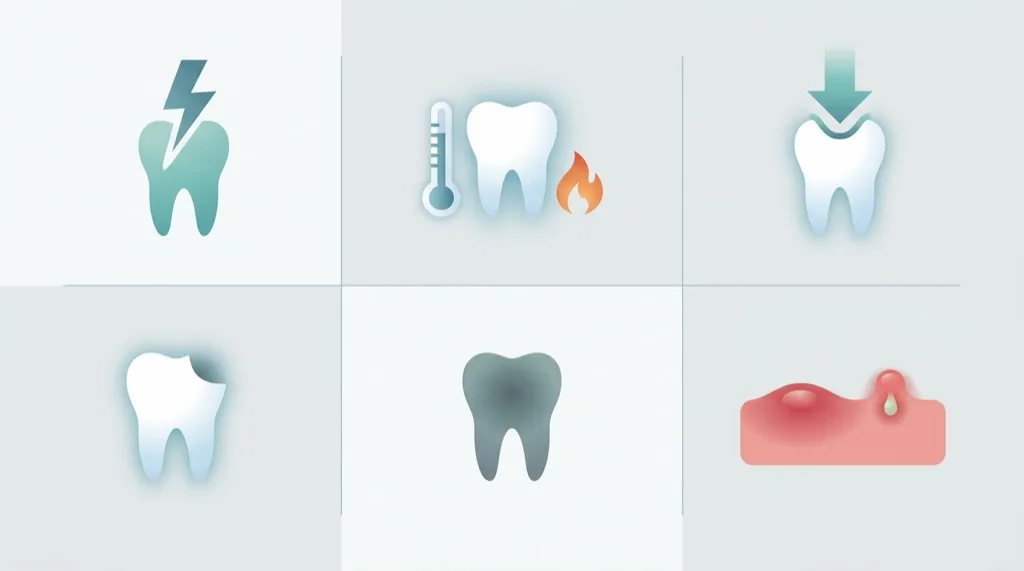
Spontaneous pain (irreversible pulpitis): A persistent, self-starting pain — often throbbing, worse at night — is the classic sign of irreversible pulpitis. The pulp is so severely inflamed that it can no longer heal itself. Root canal treatment is unavoidable at this stage.
Bite sensitivity (apical periodontitis): Pain when chewing or biting on the affected tooth indicates inflammation in the area of the root apex. The periodontal ligaments — the fibres anchoring the tooth in the bone — are inflamed and react to pressure.
Cold and heat sensitivity: Brief, quickly subsiding cold sensitivity often indicates reversible pulpitis, which can still be treated by conservative measures. If the pain persists for more than 30 seconds after removal of the stimulus, this points to irreversible pulpitis requiring root canal treatment. Strong heat sensitivity is frequently a sign of advanced inflammation.
Discoloured tooth (non-vital tooth): A progressive grey or yellow discolouration of a single tooth can indicate a dead pulp — often without any pain at all, because the nerve fibres are no longer functioning.
Swelling or sinus tract (abscess): Swelling of the gum above the affected tooth, a pimple-like sinus tract or even facial swelling are signs of an acute abscess. Immediate action is required.
Trauma (dental injury): After a dental injury — a fall, sports accident or blow — the pulp can die even without visible damage. Regular check-ups after trauma are important to monitor the condition of the pulp.
The key message: Early diagnosis and treatment significantly improve the prognosis. Do not wait with persistent symptoms — contact us at 089 95760618.
Microscopic Endodontics — The Decisive Difference
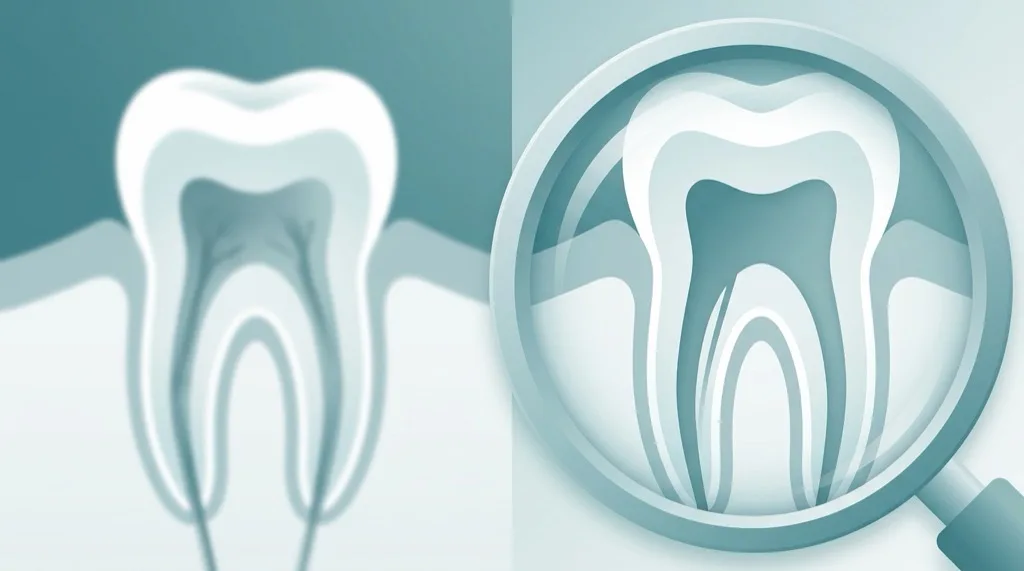
The single most important innovation in modern endodontics is the dental operating microscope. It changes everything: what the dentist sees, what they find, and ultimately, how successful the treatment is. At our practice in Munich-Oberföhring the microscope is not an optional extra — it is standard for every root canal treatment.
What the microscope achieves: At 25× magnification combined with coaxial cold-light illumination, the clinician sees details that are simply invisible to the naked eye or a basic loupe. These include:
- Hidden canals — the MB2 canal in the upper molar (the second mesiobuccal canal) is missed in up to 50% of cases when treatment is performed without a microscope. Untreated canals are the most common cause of root canal treatment failure.
- Calcified (mineralised) canals — canals narrow with age. Under the microscope even severely calcified canals can be safely located and prepared.
- Hairline cracks and fractures — a crack that jeopardises the long-term prognosis of the tooth is often undetectable without magnification. The microscope reveals it before the complex treatment begins.
- Perforations and anatomical variants — rare but clinically relevant findings that can be safely identified and managed under microscopic vision.
Success rates compared:
- Root canal treatment without magnification: approx. 70% long-term success
- Root canal treatment with operating microscope: 90–95% long-term success
This difference is clinically significant: one in five conventionally treated teeth needs to be re-treated or extracted in the medium term. The microscope cuts this risk by more than half.
Why do so few practices offer it? A high-quality dental operating microscope costs €50,000 to €100,000. This is compounded by intensive training: working under the microscope requires different hand movements and a specific learning curve. Many practices shy away from this investment. At our practice the microscope is integrated into every root canal treatment — Dr. Corinna Koderer has specialised in this very technique through multi-year curricula (Penn Tec2, Diemer Lege artis).
Root Canal Treatment in 7 Steps
Root canal treatment at our practice follows a structured, evidence-based protocol. Most treatments are completed in one to two sessions of 60–90 minutes each. Complex cases (severe infection, many canals, revision) may require two to three sessions.

1. CBCT Diagnostics — Three-Dimensional Planning
Before treatment we take a three-dimensional X-ray (CBCT — Cone Beam Computed Tomography) where needed. Unlike a conventional radiograph, the CBCT shows the exact canal anatomy, number and course of canals, periapical lesions and any fractures in all three spatial planes. This information is crucial for treatment planning — especially for complex molars, revisions or anatomical variations. For straightforward cases a high-quality 2D radiograph is often sufficient.
2. Anaesthesia — Completely Pain-Free
We use the most modern anaesthetic techniques so that you feel nothing throughout the entire treatment. For mandibular molars — the most challenging teeth for classical inferior alveolar nerve block — we use intraligamentary anaesthesia (ILA) where needed. This is administered directly into the periodontal space and provides reliable numbness even in the presence of acute inflammation. You will notice nothing except a slight pressure.
3. Kofferdam (Rubber Dam) Isolation — The Gold Standard of Endodontics
The Kofferdam (rubber dam) is a thin rubber sheet that isolates the tooth being treated from the rest of the oral cavity. It serves three critical functions: it creates a sterile working field, prevents contamination of the cleaned canals with saliva bacteria, and protects you as the patient — no accidental swallowing of irrigating solutions or instruments. The ESE (European Society of Endodontology) declares rubber dam use an indispensable standard. In our practice it is mandatory.
4. Canal Shaping — Rotary NiTi Files
Under the operating microscope all canals are shaped with rotary nickel-titanium (NiTi) files. NiTi files are flexible, follow the natural canal path without straightening artefacts, and in single-use operation are significantly safer than reused steel instruments. The motor-driven torque-controlled system minimises the fracture risk to below 1%. All canals are shaped to a uniform taper that optimises subsequent disinfection and obturation.
5. Disinfection — Ultrasonic-Activated Irrigation
Mechanical shaping alone is not enough — the canal walls are traversed by a complex network of lateral canals that no instrument can reach. We therefore irrigate with sodium hypochlorite (NaOCl) and EDTA under ultrasonic activation. The cavitation waves generated by ultrasound transport the irrigating solution into even the finest ramifications and substantially increase the disinfecting effect. In severely infected teeth a medicament dressing (calcium hydroxide) is placed for several weeks before the final filling is completed.
6. Obturation — Thermoplastic Root Canal Filling
The cleaned and disinfected canals are sealed three-dimensionally using the thermoplastic (warm) obturation technique. Gutta-percha (a biocompatible natural material) is warmed and condensed into the canals — this completely fills lateral canals and irregularities as well. This is complemented by a biocompatible sealer (e.g. calcium-silicate-based). The hermetic seal prevents re-colonisation by bacteria and is decisive for the longevity of the treatment.
7. Restoration — Adhesive Core Build-Up and Crown
After the root filling the tooth must be definitively restored as soon as possible. We place an adhesive composite core build-up that protects the tooth structure and supports the crown or filling. For posterior teeth a ceramic crown is appropriate in most cases: it protects the treated tooth from longitudinal fractures, which are an elevated risk for endodontically treated teeth without adequate cuspal coverage. For front teeth a high-quality composite filling is frequently sufficient. We will discuss the exact restoration plan with you before treatment.
Pulp Vitality Preservation — Saving Teeth Without Root Canal Treatment
Not every exposed or inflamed nerve immediately requires a complete root canal treatment. When the pulp is still alive and the inflammation is confined to a limited area, conservative procedures can preserve the vitality of the tooth — entirely without root canal treatment.
Direct pulp capping: In the case of a small, clean pulp exposure (usually due to decay or trauma) the living pulp tissue is covered directly with a bioactive material (MTA — Mineral Trioxide Aggregate or Biodentine). These calcium-silicate materials promote the formation of a dentinal bridge and allow the pulp to heal. Prerequisites: no signs of irreversible pulpitis, no abscess formation.
Indirect pulp capping: In deep decay that has not yet exposed the pulp, a thin layer of carious dentine is deliberately left in place and covered with a bioactive material. This prevents pulp exposure and simultaneously stimulates the formation of tertiary dentine.
Partial pulpotomy (Cvek pulpotomy): Only the uppermost, inflamed pulp tissue is precisely removed under the microscope; the deeper part of the pulp is preserved and sealed with MTA or Biodentine. This procedure is particularly suitable for young patients with not yet fully developed roots and for trauma cases.
When is it too late? Signs of irreversible pulpitis (spontaneous pain, prolonged pain response, periapical radiolucency on X-ray) generally rule out vitality preservation — in that case root canal treatment is the only alternative to extraction.
Dr. Corinna Koderer has studied the latest pulp vitality preservation protocols in depth during her training. Our guiding principle: "Not every exposed nerve needs root canal treatment" — we always evaluate the most conservative option first.
Revision — When a Previous Root Canal Treatment Fails
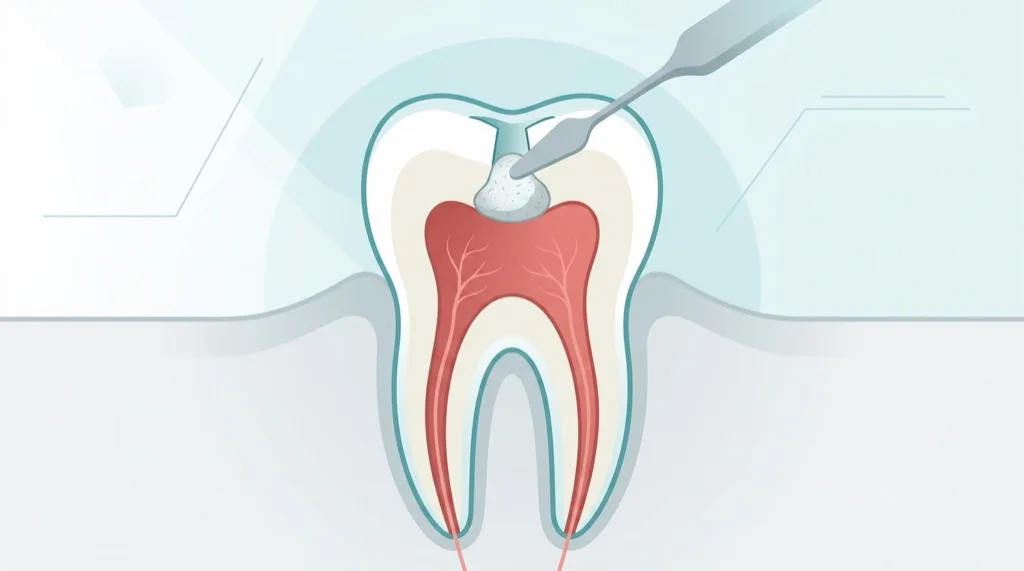
A previously performed root canal treatment is considered to have failed when persistent symptoms (pain, swelling, sinus tract) or a persistent or newly developed periapical lesion are detected on X-ray. In such cases an endodontic revision — the re-preparation and re-obturation of the canals — is often the only way to preserve the tooth long-term.
Why do root canal treatments fail? The most common causes are:
- Missed or incompletely treated canals — particularly the MB2 canal in upper molars
- Inadequate cleaning and disinfection — residual bacteria in the canal system
- Leaking obturation — gutta-percha that has shrunk or does not completely fill the canal
- Leaking coronal restoration — bacteria penetrating through poorly fitting fillings or crowns
- New decay or cracks — secondary infection of the canal system
The revision process: Under the operating microscope the old obturation (usually gutta-percha and sealer) is completely removed, all canals are located again, thoroughly cleaned and re-obturated with modern technique. Canals that were missed the first time are frequently found during revision.
Success rate of revision: With microscopic technique the success rate is 80–85% — slightly lower than for primary treatment because the canal system has already been mechanically altered. Nevertheless, revision is preferable to extraction and implantation in most cases.
When is revision no longer worthwhile? In cases of confirmed vertical root fracture, extreme bone loss or insurmountable anatomical obstacles, apicoectomy (root-end surgery) or extraction may be the better option — we will discuss this openly with you.
Apicoectomy (Root-End Surgery) — The Last Chance for the Tooth
Apicoectomy (German: Wurzelspitzenresektion, WSR) is a microsurgical procedure in which the lower portion of the tooth root (the root apex) is surgically removed and the canal is sealed from below (retrograde). It is considered when conventional revision is not possible or unlikely to succeed.
Typical indications:
- Persistent periapical lesion despite adequate endodontic treatment
- Anatomical obstacles in the canal (e.g. separated instrument, severe calcifications) that prevent orthograde revision
- Existing post and core or a valuable prosthetic restoration that should not be removed
- Persistent apical abscess in an otherwise well-restored tooth
The procedure: Under local anaesthesia the gum is reflected, the bone over the root apex is opened, and the root apex is removed under microscopic vision. The canal is cleaned from the apical end and sealed retrograde with MTA (Mineral Trioxide Aggregate) — the current gold standard for apical sealing. The wound is sutured and heals within seven to ten days as a rule. Radiographic review at six and twelve months.
Success rate: Microsurgical apicoectomy with MTA filling achieves success rates of 85–95% — a reliable option for tooth preservation when the indication is correct.
Pain-Free Root Canal Treatment — No Need to Fear the Dentist
The most common question patients ask us is: "Does root canal treatment hurt?" The answer is unambiguous: No — with modern anaesthesia and careful technique you will feel nothing during the treatment except occasional pressure.
The poor reputation of root canal treatment is rooted in history. Decades-old accounts come from an era when anaesthetics were less effective and microscopes played no role in dental practice. The fear is worse than the treatment itself — we hear this regularly from patients who finally came for treatment after years of hesitation.
Modern anaesthetic techniques we use:
- Classical inferior alveolar nerve block — proven and effective for the vast majority of cases
- Intraligamentary anaesthesia (ILA) — particularly for mandibular molars where the conventional nerve block sometimes falls short. The anaesthetic is injected directly into the periodontal space and acts quickly and reliably — even in the presence of acute inflammation
- Intraosseous anaesthesia — in rare resistant cases, direct injection into the bone for maximum reliability
What will you feel during treatment? After anaesthesia you will feel no pain — at most slight pressure during work inside the tooth. Rubber dam and microscope allow calm, precise work that places minimal stress on the tooth.
After treatment: It is normal for the tooth to be slightly pressure-sensitive during the first one to three days after treatment. Over-the-counter pain medication (ibuprofen 400–600 mg) is generally sufficient. Strong pain or swelling that increases after three days is a reason to contact us immediately.
Sedation options: For patients with severe dental anxiety we offer oral sedation by prior arrangement. This allows you to experience the treatment in a relaxed, drowsy state without being under full general anaesthesia.
If you suffer from dental anxiety, we also recommend our anxious patients page — there you will find out how we handle dental anxiety and what we can do together to make every visit more comfortable.
Our Technology for the Highest Success Rates
At our practice in Munich-Oberföhring we use only equipment and procedures whose superiority is supported by current evidence. Here is an overview of our endodontic setup:
| Technology | Specification | Clinical Benefit |
|---|---|---|
| Operating Microscope | 25× magnification, coaxial illumination | Visibility of hidden canals, cracks, calcifications; +15–25% success rate |
| CBCT (3D X-ray) | Sub-mm resolution, minimal radiation | Complete canal anatomy, periapical lesions, fracture diagnostics |
| NiTi File System | Rotary, motor-driven, single-use | Flexible, canal-conforming, no fracture risk through single-use |
| Electronic Apex Locator | Digital endometry, 3rd generation | Exact working length without additional X-rays |
| Ultrasonic-Activated Irrigation | Passive ultrasonic irrigation (PUI) | Disinfection in lateral canals and isthmic connections as well |
| Thermoplastic Obturation | Warm vertical condensation | 3D sealing of all canal ramifications, denser than cold filling |
This combination corresponds to the current recommendations of the ESE (European Society of Endodontology) and the DGZ (Deutsche Gesellschaft für Zahnerhaltung — German Society for Restorative Dentistry) for high-quality endodontics.

Success Rates and Scientific Evidence
Endodontics is one of the most thoroughly researched disciplines in dentistry. All success rate data are based on published clinical studies and the guidelines of the ESE (European Society of Endodontology).
Success rates at a glance:
- Primary treatment with operating microscope: 90–95% long-term success (≥4 years)
- Primary treatment without magnification: approx. 70% long-term success
- Revision with operating microscope: 80–85% long-term success
- Microsurgical apicoectomy with MTA: 85–95% long-term success
- Long-term tooth retention: 10–20+ years with adequate restoration and regular follow-up
Definition of "success": Clinically, a treatment is considered successful when, after at least four years, there are no symptoms, the periapical lesion has healed radiologically, and the tooth fulfils its function.
Studies show that the coronal restoration — the filling or crown after root canal treatment — is just as decisive for long-term prognosis as the quality of the endodontic treatment itself. A leaking coronal seal can re-contaminate the canal system and render even the best root filling ineffective. This is why we insist on prompt definitive restoration after root canal treatment.
Cost of Root Canal Treatment
The cost of root canal treatment depends on which techniques are used and how complex the tooth is. In Germany a distinction is made between the statutory health insurance (GKV) basic service (BEMA) and private additional services (GOZ) that enable a higher quality of treatment.
| Service | GKV (BEMA) | Co-payment (GOZ) | Why worthwhile? |
|---|---|---|---|
| Basic treatment | Covered by GKV | €0 | Standard care without magnification |
| Electronic apex locator | Not included | €30–60 | Exact canal length, fewer X-rays |
| Operating microscope | Not included | €200–400 | 25× magnification, +15–25% success rate |
| Rotary NiTi instrumentation | Not included | €80–150 | Gentler, more complete cleaning |
| Ultrasonic-activated irrigation | Not included | €40–80 | Better disinfection of lateral canals |
| Thermoplastic obturation | Not included | €60–120 | Denser filling than cold technique |
| CBCT (3D X-ray) | Not included | €80–200 | Complex anatomy, revisions |
Typical total co-payment: For primary treatment with a full modern protocol (microscope, NiTi, ultrasound, thermoplastic filling) GKV patients should expect a co-payment of approx. €150–600 per tooth — depending on the number of canals and complexity. A revision typically costs €400–900 in co-payment; a microsurgical apicoectomy €300–600.
For comparison: An implant including abutment and crown costs €2,000–4,000 — mostly without GKV reimbursement and involving a surgical procedure. The co-payment for modern root canal treatment is therefore a very cost-effective investment in tooth preservation.
Before treatment begins we will provide you with a transparent treatment and cost plan so you know exactly what to expect. No hidden costs.
Aftercare and Longevity
A well-performed root canal treatment is not an endpoint — it is the beginning of a new life cycle for the tooth. With the right aftercare and timely restoration, an endodontically treated tooth can remain trouble-free for many decades.
Immediately after treatment (first 1–3 days): The tooth may be slightly sensitive to pressure — this is a normal irritation response of the periapical tissue. Over-the-counter pain medication (ibuprofen 400–600 mg, three times daily as needed) is generally completely sufficient. Chew on the other side if possible until the definitive restoration has been placed.
When should you contact us? If pain or swelling increases rather than subsides after three days, if visible swelling develops, or if you develop a fever — please contact us immediately at 089 95760618.
Definitive restoration — as soon as possible: The most important step after root canal treatment is timely placement of a definitive restoration. We recommend an adhesive composite core build-up within 2–4 weeks. For posterior teeth a full-ceramic crown is appropriate in most cases, as non-vital teeth are more brittle and carry an increased fracture risk without cuspal protection. For front teeth a high-quality composite filling or veneer is often sufficient.
Radiographic reviews: Six months after treatment we take a review radiograph to assess healing of the periapical lesion. If the findings are unremarkable, an annual radiographic check as part of routine examination is sufficient thereafter.
Longevity: With a completely sealed restoration and regular preventive care, endodontically treated teeth last 10–20+ years in the majority of cases — often a lifetime.
Your Endodontics Specialists
At our practice in Munich-Oberföhring you benefit from a rare constellation: two specialists under one roof who complement each other and together cover the complete spectrum of modern endodontics — from pulp vitality preservation through primary treatment and revision to surgical apicoectomy and, where necessary, implantology.
Dr. Corinna Koderer — Endodontics Specialist
Dr. Koderer is our specialist in microscopic endodontics. Her training encompasses the most demanding endodontic curricula in the German-speaking world:
- Tec2 Next-Level-Endo Curriculum, University of Pennsylvania (2025+)
- Tec2 Endodontie Curriculum, University of Pennsylvania (2025)
- Lege artis Endodontie bei Dr. Josef Diemer (2023)
- Promotion magna cum laude, MKG Chirurgie, Universität Würzburg (2022)
- Staatsexamen Note 1, Julius-Maximilians-Universität Würzburg (2019)
"Every tooth deserves a chance. With the microscope and modern techniques we can today save teeth that were once considered hopeless."
Dr. Christina Dickel — Practice Principal
Dr. Dickel brings over 13 years of clinical experience and a broad range of additional qualifications:
- Curriculum Implantologie, Deutsche Gesellschaft für Implantologie DGI (2014)
- Curriculum Ästhetische Zahnheilkunde, DGÄZ (2015)
- Curriculum Parodontologie, DG PARO (2016)
- Staatsexamen Zahnmedizin, Heinrich-Heine-Universität Düsseldorf (2012)
As practice principal, Dr. Dickel coordinates the overall treatment — from first contact through endodontics to prosthetic restoration. If a tooth cannot be saved despite all efforts, she can transition seamlessly into implantology — everything under one roof, without referring patients to another practice.
Important cross-disciplinary topics we address together with you:
- Periodontology — endo-perio lesions require coordinated treatment of both structures
- Caries treatment — deep decay is the most common cause of pulpitis
- Anxious patients — we take your anxiety seriously and find a way forward together

Kosten im Überblick
| Leistung | Preisrahmen | Hinweis |
|---|---|---|
| Basic treatment (BEMA) | GKV covered | Standard care without magnification or rotary instrumentation |
| Electronic apex locator | €30 - €60 | Exact canal length determination, fewer radiographs required |
| Operating microscope | €200 - €400 | 25× magnification for highest precision and success rate |
| Rotary NiTi instrumentation | €80 - €150 | Flexible single-use files for gentle, complete canal cleaning |
| Ultrasonic-activated irrigation | €40 - €80 | More effective disinfection including lateral canals |
| Thermoplastic obturation | €60 - €120 | Warm fill technique for dense, three-dimensional sealing |
| CBCT (3D X-ray) | €80 - €200 | Three-dimensional imaging for complex anatomy or revisions |
| Primary treatment total (co-payment) | €150 - €600 | Typical total co-payment per tooth for modern endodontics |
| Revision (co-payment) | €400 - €900 | Re-treatment when initial care was inadequate |
| Microsurgical apicoectomy (co-payment) | €300 - €600 | Microsurgical root-end surgery with MTA sealing |
Basic treatment (BEMA)
GKV covered
Standard care without magnification or rotary instrumentation
Electronic apex locator
€30 - €60
Exact canal length determination, fewer radiographs required
Operating microscope
€200 - €400
25× magnification for highest precision and success rate
Rotary NiTi instrumentation
€80 - €150
Flexible single-use files for gentle, complete canal cleaning
Ultrasonic-activated irrigation
€40 - €80
More effective disinfection including lateral canals
Thermoplastic obturation
€60 - €120
Warm fill technique for dense, three-dimensional sealing
CBCT (3D X-ray)
€80 - €200
Three-dimensional imaging for complex anatomy or revisions
Primary treatment total (co-payment)
€150 - €600
Typical total co-payment per tooth for modern endodontics
Revision (co-payment)
€400 - €900
Re-treatment when initial care was inadequate
Microsurgical apicoectomy (co-payment)
€300 - €600
Microsurgical root-end surgery with MTA sealing
Private health insurance and supplementary dental insurance generally cover the full cost of modern endodontics. GKV patients receive a detailed cost plan before treatment begins.
Instalment payment by individual arrangement possible. Please ask us.
Risiken und Sicherheit
Root canal treatment is a safe, well-established procedure. As with any medical intervention there are risks, which we minimise through modern technology and experience.
Instrument fracture (file separation)
Rare (<1% with NiTi)
NiTi single-use files, motor-driven torque control, microscope for retrieval
Perforation (root wall penetration)
Very rare
Microscopic vision, CBCT planning, MTA repair if needed
Persistent infection
5–10% (with microscope <5%)
Ultrasonic irrigation, medicament dressing, revision if needed
Post-operative pain
Common (1–3 days, mild)
OTC medication, resolves spontaneously
Tooth fracture (long-term)
Possible without crown
Timely definitive restoration, crown for posterior teeth
Tooth discolouration
Occasional
Internal bleaching possible, crown or veneer
Our combination of operating microscope, CBCT, NiTi single-use files and ultrasonic-activated irrigation reduces each of these risks to a minimum. The success rate is 90–95%.
Qualifikationen und Zertifikate
2025+
Tec2 Next-Level-Endo Curriculum
University of Pennsylvania
2025
Tec2 Endodontie Curriculum
University of Pennsylvania
2024
Curriculum Implantologie
Deutsche Gesellschaft für Implantologie (DGI)
2023
Lege artis Endodontie
Dr. Josef Diemer
2022
Promotion (Dr. med. dent.) magna cum laude
MKG Chirurgie, Universität Würzburg
2019
Staatsexamen Zahnmedizin (Note 1)
Julius-Maximilians-Universität Würzburg
—
2012–present
Over 13 years of clinical experience
2016
Curriculum Parodontologie
DG PARO
2015
Curriculum Ästhetische Zahnheilkunde
DGÄZ
2014
Curriculum Implantologie
Deutsche Gesellschaft für Implantologie (DGI)
2012
Staatsexamen Zahnmedizin
Heinrich-Heine-Universität Düsseldorf
Häufige Fragen
Ready to take your first step?
Book an appointment for a personal consultation at our practice in Munich Oberföhring.

