Inhaltsverzeichnis
What Is Periodontitis?
Periodontitis — commonly referred to as "gum disease" — is a chronic inflammatory condition affecting the tooth-supporting structures (periodontium). It affects not only the gums but also the jawbone, root cementum, and the fibres that anchor the tooth in the bone. Left untreated, periodontitis leads to the breakdown of these structures and ultimately to tooth loss.
The condition is widespread: approximately 50% of all adults over 40 are affected. Periodontitis is the most common cause of tooth loss in adults — more so than tooth decay. The insidious aspect: it often progresses painlessly for a long time and is therefore frequently detected only at an advanced stage.
At our dental practice in Munich-Oberföhring, we rely on early diagnosis using a cone beam CT (CBCT) and modern treatment methods to preserve your teeth for the long term.
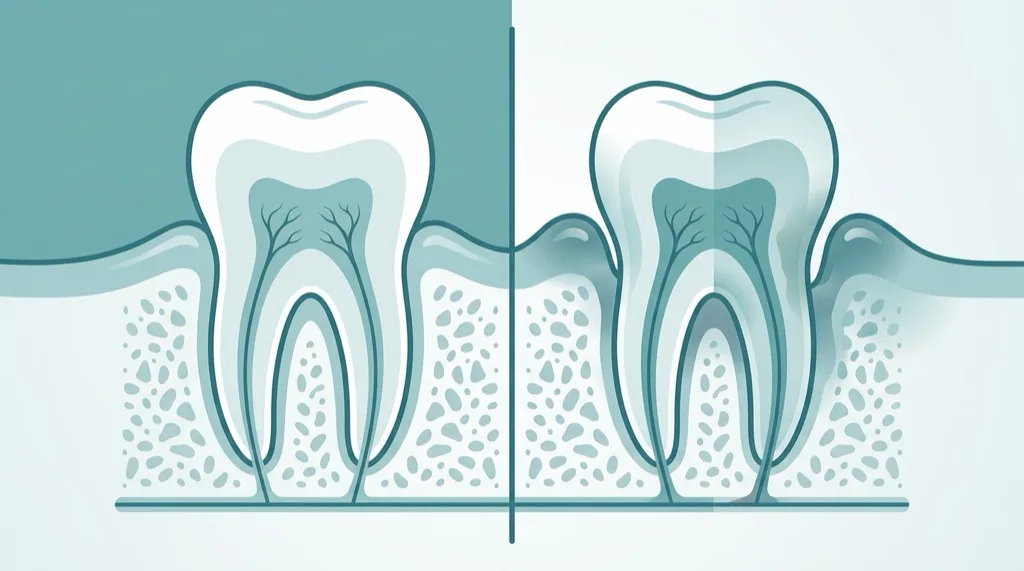
Gingivitis vs. Periodontitis — the Difference
Gingivitis (gum inflammation) is the precursor to periodontitis. It is confined to the gums: they appear red, swollen, and bleed when brushing. The good news: gingivitis is fully reversible. With a professional dental cleaning (PDC) and improved oral hygiene at home, the inflammation heals completely.
If gingivitis is left untreated, it can progress to periodontitis. The inflammation then extends to the jawbone — deepened periodontal pockets form, and bone is irreversibly lost. This transition is the critical moment: what was still easy to stop at the gingivitis stage now requires systematic treatment for periodontitis.
Periodontitis Is Treatable
The most important message: periodontitis is treatable. While bone that has been lost can only be partially regenerated, the disease can be halted and controlled. With modern anti-infective therapy, regenerative procedures, and consistent follow-up care (UPT), over 95% of patients keep their teeth long-term.
The earlier treatment begins, the better the prognosis. If you notice symptoms or are unsure — get examined. A simple pocket depth measurement is sufficient to assess the condition of your periodontal apparatus.
Recognising Symptoms & Understanding Stages
Periodontitis often develops gradually. Watch for these warning signs:
- Bleeding gums when brushing or eating hard foods
- Red or swollen gums
- Bad breath (halitosis) that does not go away despite good oral hygiene
- Gum recession — teeth appear longer
- Sensitive tooth necks with hot, cold, or sweet foods
- Loose teeth or changes in tooth position
- Pus discharge from the periodontal pockets
- Unpleasant taste in the mouth
Important: Even one of these symptoms may indicate periodontitis. Bleeding gums are not normal — not even "just a little".
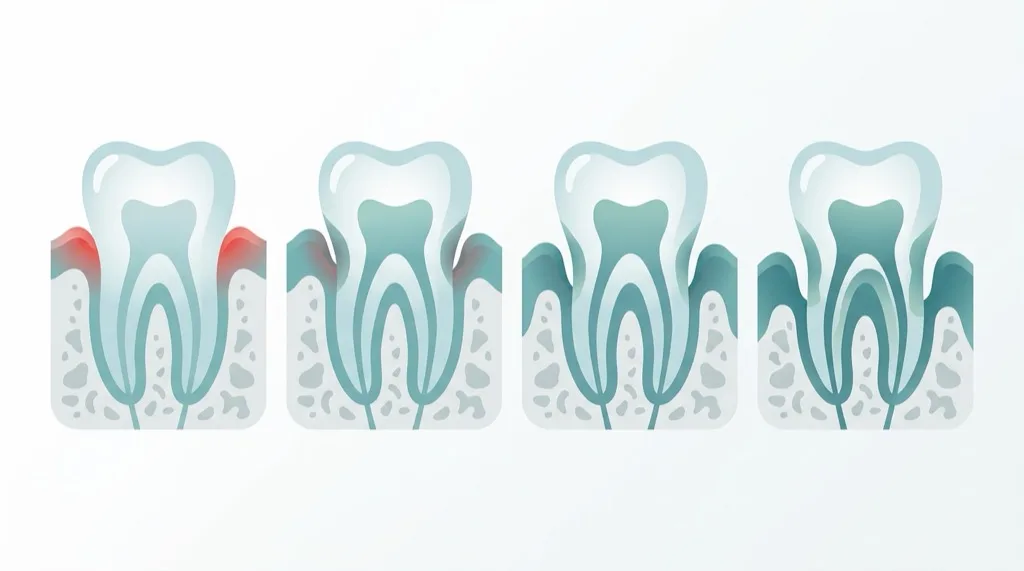
The European Federation of Periodontology (EFP) and the American Academy of Periodontology (AAP) introduced a new classification in 2018 that categorises periodontitis by severity (stage) and rate of progression (grade):
Stages (Severity):
| Stage | CAL (Attachment Loss) | Bone Loss (Radiographic) | Typical Features |
|---|---|---|---|
| I (Mild) | 1–2 mm | Coronal third (<15%) | Bleeding gums, mild redness, max. pocket depth ≤4 mm |
| II (Moderate) | 3–4 mm | Coronal third (15–33%) | Gum recession, bad breath, pocket depth ≤5 mm |
| III (Severe) | ≥5 mm | Up to middle third of root | Loose teeth, ≤4 teeth lost, deep pockets ≥6 mm |
| IV (Very Severe) | ≥5 mm | Beyond middle third (apical) | ≥5 teeth lost, bite problems, chewing impairment |
Grades (Rate of Progression):
| Grade | Progression | Risk Factors |
|---|---|---|
| A (Slow) | No loss over 5 years | Non-smoker, no diabetes |
| B (Moderate) | Loss proportional to age | Smoker <10 cigarettes/day |
| C (Rapid) | Loss disproportionate to age | Smoker >10 cigarettes/day or diabetes |
This classification helps us plan your treatment individually and assess the prognosis realistically. At the initial examination, we determine the stage and grade based on pocket measurements, X-rays, and your medical history.
Causes and Risk Factors
The main cause of periodontitis is bacterial biofilm (plaque) on tooth surfaces and below the gum line. More than 700 bacterial species live in the oral cavity — most are harmless. However, certain periodontal pathogens (such as Porphyromonas gingivalis or Aggregatibacter actinomycetemcomitans) can trigger an excessive immune response that destroys the body's own tissue.
Whether and how quickly gingivitis progresses to periodontitis depends on several risk factors:
- Smoking — the greatest modifiable risk factor. Smokers are 3–6 times more likely to develop the disease and respond less well to treatment.
- Diabetes mellitus — especially with poorly controlled blood sugar (bidirectional relationship)
- Genetic predisposition — up to 50% of disease risk is genetically determined
- Stress — weakens the immune system and promotes inflammatory processes
- Hormonal changes — pregnancy, puberty, menopause
- Medications — certain blood pressure medications, immunosuppressants, antiepileptics
- Poor oral hygiene — plaque accumulation as a prerequisite
Can Periodontitis Be Prevented?
Yes — and prevention is considerably easier than treatment. The most important measures:
- Thorough home oral hygiene — brush twice daily plus use interdental brushes or floss
- Regular professional dental cleaning (PDC) — at least twice a year, more frequently for those at higher risk
- Not smoking — the most effective single protective factor
- Good diabetes management — keep HbA1c below 7%
- Regular check-ups — PSI screening 1–2 times a year
Professional dental cleaning is a central element of periodontitis prevention. It removes bacterial biofilm even in areas that your toothbrush cannot reach.
Periodontitis & General Health
Periodontitis is more than a condition of the mouth. The chronic inflammation releases bacteria and inflammatory mediators that travel through the bloodstream to the entire body. Research in recent years has established clear links between periodontitis and several systemic diseases.
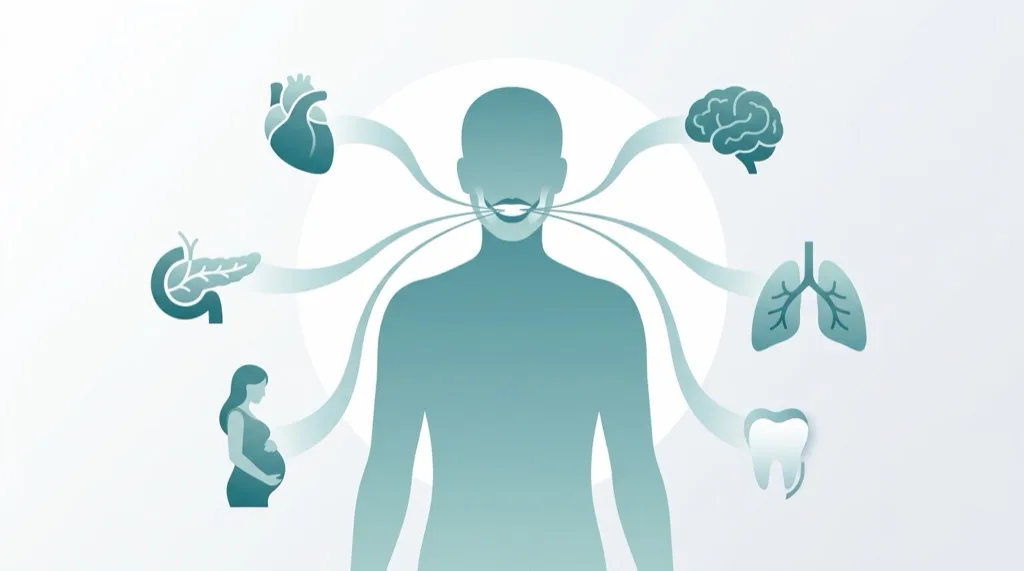
Diabetes Mellitus
The relationship between diabetes and periodontitis is bidirectional: diabetes increases the risk of periodontitis threefold, and conversely, untreated periodontitis worsens blood sugar control. Studies show that successful periodontal treatment can reduce HbA1c by 0.3–0.4% — comparable to the effect of an additional diabetes medication.
Cardiovascular Disease
Periodontitis patients have an elevated risk of heart attack and stroke. Chronic inflammation raises CRP (C-reactive protein) levels in the blood and promotes atherosclerosis. Periodontal bacteria have been detected in atherosclerotic plaques. There is also a risk of endocarditis (heart valve inflammation), particularly in patients with pre-damaged heart valves.
Pregnancy
Untreated periodontitis during pregnancy increases the risk of preterm birth and low birth weight. Inflammatory mediators can trigger premature labour. Periodontal treatment during pregnancy is safe and is even recommended — ideally in the second trimester.
Respiratory Conditions
Periodontal bacteria can be inhaled and contribute to pneumonia (aspiration pneumonia) — especially in elderly or immunocompromised patients. Good oral health has been shown to reduce the risk of respiratory infections.
Rheumatoid Arthritis
Rheumatoid arthritis and periodontitis share similar inflammatory mechanisms. Studies show that periodontitis patients are more likely to develop rheumatoid arthritis and vice versa. Treating periodontitis can also have a positive effect on joint symptoms.
Treatment Process Step by Step
Periodontal treatment follows a proven, systematic process in accordance with the guidelines of the Deutsche Gesellschaft für Parodontologie (DG PARO). Each step builds on the previous one — this is how we achieve the best possible prognosis for your teeth.
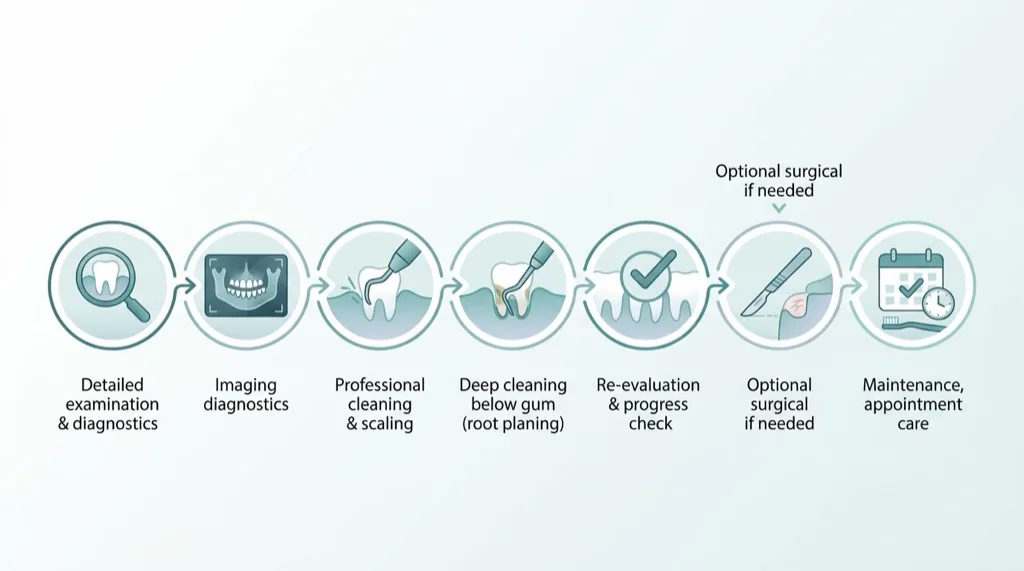
1. Initial Consultation & Periodontal Assessment
At the first appointment, we carry out a comprehensive periodontal examination. This includes the PSI (Periodontal Screening Index), a full pocket depth measurement at 6 points per tooth, and assessment of tooth mobility and gum recession. The PSI is covered by statutory health insurance and is recommended twice a year as an early detection examination.
2. 3D Diagnostics with CBCT
With our cone beam CT (CBCT), we create three-dimensional images of your jaw. Unlike a conventional X-ray, we can assess bone loss to the millimetre — including in hard-to-see areas such as furcations (root bifurcations). CBCT diagnostics offer a decisive advantage for precise treatment planning.
3. Pre-Treatment (PDC & Oral Hygiene Instruction)
Prior to the actual periodontal therapy, pre-treatment takes place: a professional dental cleaning (PDC) and individual oral hygiene instruction. You will learn how to effectively remove biofilm at home — because your contribution is crucial to treatment success.
4. Anti-Infective Therapy (Scaling & Root Planing)
The core of treatment: under local anaesthesia, all periodontal pockets are thoroughly cleaned. Using ultrasonic instruments and fine hand instruments (curettes), we remove bacterial biofilm, tartar (calculus), and inflamed tissue from the pockets. At the same time, the root surfaces are smoothed (root planing) so that biofilm is less able to recolonise. We typically treat one jaw per session.
5. Re-Evaluation after 3 Months
Three months after anti-infective therapy, we measure all pockets again. In most cases, there is a clear improvement: pockets are shallower and inflammation has subsided. Based on the results, we decide whether further measures are needed or whether we can move directly into follow-up care (UPT).
6. Surgical Therapy (if required)
For remaining deep pockets (≥6 mm), surgical therapy may be necessary. The gum tissue is reflected (flap surgery) to clean the root surfaces under direct vision. For suitable bone defects, we use regenerative procedures — for example Emdogain® (enamel matrix proteins) or GTR membranes — to partially regenerate lost bone.
7. Transition to UPT (Supportive Periodontal Therapy)
After active therapy is complete, lifelong follow-up care begins: the UPT. It is the foundation for long-term success. Without regular UPT, periodontitis almost always returns. More on this in the section Follow-Up Care & UPT.
Modern Treatment Methods
In our practice, we combine proven procedures with modern technology. Our goal: treatment that is as gentle, effective, and predictable as possible. Here is an overview of the methods we use:
| Method | Application | Advantage | In Our Practice |
|---|---|---|---|
| CBCT 3D Diagnostics | Bone assessment | Millimetre-precise planning | ✓ |
| Piezo Ultrasonic | Tartar removal | Particularly gentle | ✓ |
| Diode Laser | Pocket disinfection | Bacterial reduction >99% | ✓ |
| Emdogain® | Bone regeneration | Natural healing | ✓ |
| PerioChip® | Local antibiotic therapy | Targeted, without systemic side effects | ✓ |

CBCT (Cone Beam Computed Tomography)
Our CBCT delivers three-dimensional images with a resolution of up to 0.1 mm. This allows us to precisely assess bone defects, furcation involvement, and vertical bone loss — the basis for precise treatment planning and the decision of whether regenerative procedures are likely to be successful.
Piezo Ultrasonic
Modern piezo ultrasonic instruments remove tartar and biofilm particularly gently. The high-frequency vibrations loosen deposits without damaging the sensitive root surface. At the same time, the irrigation ensures continuous flushing and cleaning of the pockets.
Laser-Assisted Therapy
The diode laser complements the mechanical cleaning of periodontal pockets. The laser light reaches areas that instruments cannot access and reduces the bacterial load by over 99%. At the same time, laser treatment promotes wound healing and tissue regeneration. The procedure is low-pain and shortens healing time.
GTR (Guided Tissue Regeneration)
For suitable bone defects, we use barrier membranes that encourage bone tissue to grow into the defect while preventing the faster-growing gum tissue from filling it. This allows new bone to form in the protected area.
Emdogain® (Enamel Matrix Proteins)
Emdogain® contains enamel matrix proteins that mimic the natural developmental process of the periodontium. Applied to the cleaned root surface, they stimulate the regeneration of bone, root cementum, and fibres. Emdogain® achieves particularly good results with vertical bone defects.
PerioChip® (Local Antibiotic Therapy)
PerioChip® is a small gelatin chip that delivers chlorhexidine directly into the periodontal pocket — over a period of 7–10 days. It is placed in persistently deep pockets after scaling and reduces the bacterial load precisely at the site of inflammation, without systemic side effects.
Costs and Insurance (PAR-Richtlinie)
Thanks to the PAR-Richtlinie, which has been in effect since July 2021, insurance coverage for periodontitis patients has fundamentally improved. Systematic periodontal therapy has since been a benefit of statutory health insurance (GKV). Here is a transparent overview:
| Treatment | Cost | Covered by Insurance |
|---|---|---|
| Periodontal assessment (PSI) | Covered by insurance | ✓ GKV 2x/year |
| Pre-treatment (PDC + OHI) | 80–160 EUR | Partial (subsidies) |
| Anti-infective therapy (per jaw) | 300–600 EUR | ✓ GKV since PAR-Richtlinie |
| Surgical therapy (per sextant) | 200–500 EUR | Partial GKV |
| Regenerative therapy (Emdogain®) | 300–800 EUR | Private service |
| UPT session | 80–150 EUR | ✓ GKV (PAR-Richtlinie, 2 years) |
What the PAR-Richtlinie (since 2021) means:
Since July 2021, statutory health insurance covers the costs of systematic periodontal treatment. This includes:
- Diagnostics — PSI and periodontal assessment
- Anti-infective therapy — Scaling & Root Planing (subgingival debridement)
- UPT — Supportive Periodontal Therapy over 2 years (months 3, 6, 12, 18, 24)
Requirement: An AIT application (application for approval of anti-infective therapy) must be submitted to and approved by your health insurance provider. We submit this application on your behalf — the process typically takes 2–3 weeks.
After 2 years: GKV coverage for UPT ends after 24 months. We then recommend continuing follow-up care as a private service — your dental health is worth the investment.
Further information about the PAR-Richtlinie is available from the Kassenzahnärztliche Bundesvereinigung (KZBV).
Private insurance: Privately insured patients receive reimbursement of 80–100% of all services depending on their plan — including regenerative procedures (Emdogain®, GTR). We provide you with a detailed treatment and cost plan to submit to your insurer.

Follow-Up Care & Supportive Periodontal Therapy (UPT)
UPT is the most important element of periodontal treatment — because the real challenge begins after active therapy. Periodontitis is a chronic condition: without regular follow-up care, it almost always returns.
What happens at a UPT session?
- Pocket measurement — checking whether pocket reduction remains stable
- Biofilm removal — professional cleaning of all periodontal pockets
- Re-instruction — refresher on home oral hygiene technique
- Inflammation monitoring — bleeding on probing (BOP) as an early warning system
- X-ray check — when needed, to verify bone status
UPT Schedule:
- In the first year: every 3 months
- When stable: every 3–6 months (individually adjusted)
- Lifelong: UPT should not end — periodontitis requires ongoing management
Long-term prognosis: The 30-year study by Axelsson and Lindhe demonstrates impressively: patients with regular follow-up care retain over 95% of their teeth. Without follow-up care, tooth loss is significantly higher. UPT is therefore the best investment in your dental health.
The GKV covers UPT costs for the first 2 years under the PAR-Richtlinie. We then strongly recommend continuing follow-up care as a private service. In our practice, we offer you an individual UPT concept tailored to your personal risk profile.

Risks and Prognosis
Periodontal treatment is a well-established, safe procedure with an excellent prognosis. The most common side effects are part of the normal healing process and a sign that treatment is working:
- Post-operative sensitivity — common and normal, subsides after 1–3 days. Pain relief (ibuprofen) as needed.
- Gum recession after therapy — common. The swelling subsides and the gums tighten — teeth may temporarily appear "longer".
- Exposed tooth necks — occasional. Treatable with desensitising varnishes or fluoride application.
- Temporary tooth mobility — rare. Stabilises once the bone has healed.
- Recurrence with inadequate follow-up — possible, but preventable. Regular UPT reliably prevents relapse.
In our practice, we minimise risks through precise CBCT diagnostics, gentle ultrasonic and laser technology, and an individual UPT follow-up concept. Every treatment is tailored to your personal situation.
Your Treating Dentist — Dr. Christina Dickel
At my practice in Munich-Oberföhring, I treat periodontitis with a clear focus on modern technology and personalised care. My approach: precise diagnostics with CBCT, gentle therapy with ultrasound and laser, and close follow-up care tailored to your individual risk profile.
I have been treating patients with periodontitis for over 13 years — from mild gingivitis to advanced cases requiring bone regeneration. In 2016, I completed the Curriculum Parodontologie of the Deutsche Gesellschaft für Parodontologie (DG PARO), which provides in-depth advanced training in all aspects of periodontal therapy.
My goal is to preserve your natural teeth for as long as possible. With modern technology, a clear treatment plan, and your commitment to home care, we create the best conditions together for achieving this.
My technical equipment for periodontal treatment:
- CBCT 3D diagnostics — for millimetre-precise bone assessment
- Diode laser — for gentle pocket disinfection
- Piezo ultrasonic — for tissue-sparing scaling
- Digital charting — for seamless progress monitoring
If you have questions or would like an examination — book an appointment. An initial periodontal examination takes approximately 30 minutes and gives us a clear picture of your situation.
Kosten im Überblick
| Leistung | Preisrahmen | Hinweis |
|---|---|---|
| Periodontal assessment (PSI) | Covered by insurance | GKV 2x/year as early detection examination |
| Pre-treatment (PDC + OHI) | 80 - 160 EUR | Professional dental cleaning and oral hygiene instruction |
| Anti-infective therapy (per jaw) | 300 - 600 EUR | Scaling & Root Planing, subgingival debridement |
| Surgical therapy (per sextant) | 200 - 500 EUR | Flap surgery for deep pockets |
| Regenerative therapy (Emdogain®) | 300 - 800 EUR | Enamel matrix proteins for bone regeneration |
| UPT session | 80 - 150 EUR | Follow-up care every 3–6 months |
Periodontal assessment (PSI)
Covered by insurance
GKV 2x/year as early detection examination
Pre-treatment (PDC + OHI)
80 - 160 EUR
Professional dental cleaning and oral hygiene instruction
Anti-infective therapy (per jaw)
300 - 600 EUR
Scaling & Root Planing, subgingival debridement
Surgical therapy (per sextant)
200 - 500 EUR
Flap surgery for deep pockets
Regenerative therapy (Emdogain®)
300 - 800 EUR
Enamel matrix proteins for bone regeneration
UPT session
80 - 150 EUR
Follow-up care every 3–6 months
Statutory insurance patients: anti-infective therapy and UPT have been covered services since 2021. Regenerative procedures (Emdogain®, GTR) are private services. Private insurers reimburse 80–100% of all services depending on the plan.
For extensive treatments involving regenerative procedures, we offer payment by instalments. Contact us — we will create a transparent treatment and cost plan for you.
Risiken und Sicherheit
Periodontal treatment is a well-established, safe procedure with an excellent prognosis. The most common side effects are part of the normal healing process:
Post-operative sensitivity
Common (normal)
Subsides after 1–3 days; pain relief as needed
Gum recession after therapy
Common
Normal course of healing — swelling subsides and gums tighten
Exposed tooth necks
Occasional
Desensitising treatment, fluoride varnish
Temporary tooth mobility
Rare
Stabilises once the bone has healed
Recurrence with inadequate follow-up
Possible
Regular UPT reliably prevents relapse
In our practice, we minimise risks through precise CBCT diagnostics, gentle ultrasonic and laser technology, and an individual UPT follow-up concept. Every treatment is tailored to your personal situation.
Qualifikationen und Zertifikate
2012
State Examination in Dentistry
Heinrich-Heine-Universität Düsseldorf
2016
Curriculum Parodontologie
Deutsche Gesellschaft für Parodontologie (DG PARO)
CBCT Certification
Cone Beam Computed Tomography
Advanced Training in Laser-Assisted Periodontal Therapy
Over 13 years of experience in periodontal treatment
Häufige Fragen
Ready to take your first step?
Book an appointment for a personal consultation at our practice in Munich Oberföhring.

