Inhaltsverzeichnis
What is Periodontitis?
Periodontitis is a chronic inflammatory infectious disease of the periodontium, triggered by bacterial biofilms (plaque) below the gum line. The term is often colloquially equated with "bleeding gums" — but that is an oversimplification. Periodontitis systematically destroys the entire tooth-supporting apparatus: the gingiva, periodontal ligament, alveolar bone, and the fibers that anchor the tooth in the bone.
The numbers speak clearly: periodontitis is the most common cause of tooth loss in adults — even ahead of tooth decay. More than 50% of all adults over 40 in Germany are affected by periodontitis requiring treatment, and many are not even aware of it. This is because the disease progresses painlessly and insidiously for a long time, until tooth loss threatens.
The distinction between gingivitis and periodontitis is crucial: gingivitis (gum inflammation) affects only the gingival tissue and is completely reversible with consistent treatment and improved oral hygiene. However, once the inflammation has spread to the alveolar bone and bone loss has occurred, we are dealing with periodontitis — a condition that is treatable and controllable, but cannot be completely reversed.
The insidious aspect: most patients only notice the disease at an advanced stage because pain is absent for a long time. Regular check-ups are therefore essential. At our dental practice in Munich-Oberföhring, we perform a Periodontal Screening Index (PSI) at every recall appointment — the simplest and fastest method to detect periodontitis at an early stage.
If you suspect you may be affected, do not hesitate: call us at 089 95760618 or book an appointment online. Early detection is the most effective weapon against periodontitis.
Do You Have Periodontitis? — The Self-Check
Periodontitis develops gradually — but there are warning signs you can recognise yourself. The following self-check helps you assess whether you should schedule a dental appointment. Please note: this check does not replace a dental examination. Only probing depth measurements and an X-ray can reliably diagnose periodontitis.
Check which of the following symptoms apply to you:
- Bleeding gums when brushing or eating — Healthy gums do not bleed. Even occasional bleeding is not a "normal state" but an alarm signal for inflammation.
- Reddened, swollen gums — Healthy gums are light pink to salmon-coloured and firmly attached. Redness and swelling indicate active inflammation.
- Gum recession — your teeth look longer than before — When tooth necks become exposed, it is a sign that the gums are receding. This may indicate periodontitis or aggressive tooth brushing.
- Persistent bad breath (halitosis) — Bacteria in deep periodontal pockets produce sulphur compounds responsible for chronic bad breath. If bad breath does not disappear despite good oral hygiene, periodontitis should be ruled out.
- Sensitive tooth necks — Exposed tooth necks often react painfully to cold, hot or sweet foods and drinks. This symptom arises when the gums have receded due to inflammation.
- Loose teeth or tooth migration — If teeth feel as though they are wobbling, or their position has changed, the periodontium is already significantly damaged. This is an urgent warning signal.
- Pus formation between tooth and gum — Visible pus or an unpleasant taste in the mouth (especially in the morning) can indicate a periodontal abscess — an acute finding that requires immediate treatment.
- Changed bite — teeth no longer fit together properly — If your bite has changed or dental restorations (bridges, crowns) suddenly fit differently, tooth migration due to periodontitis may be the cause.
Your assessment:
1–2 symptoms: Possible gingivitis or early periodontitis. A dental check-up is advisable.
3 or more symptoms: The probability of periodontitis requiring treatment is high. Make an appointment promptly by calling 089 95760618. The earlier we treat, the better your prognosis and the more tooth structure can be preserved.
At our practice in Munich-Oberföhring, we carry out comprehensive periodontal diagnostics: probing depth measurements at all 6 measurement points per tooth, digital X-rays, bleeding indices and assessment of the oral microbiome. This examination forms the basis for an individualised treatment plan.
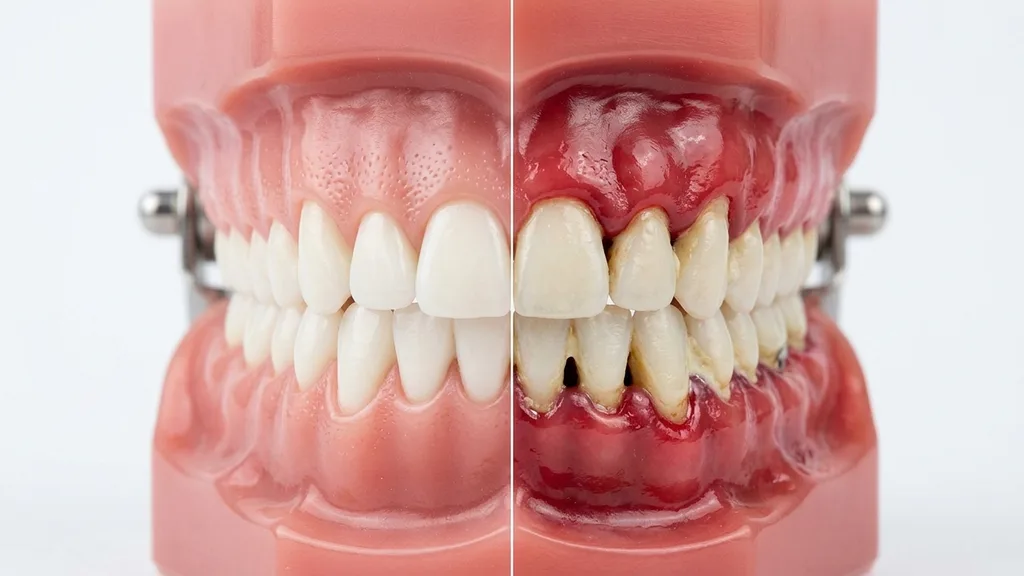
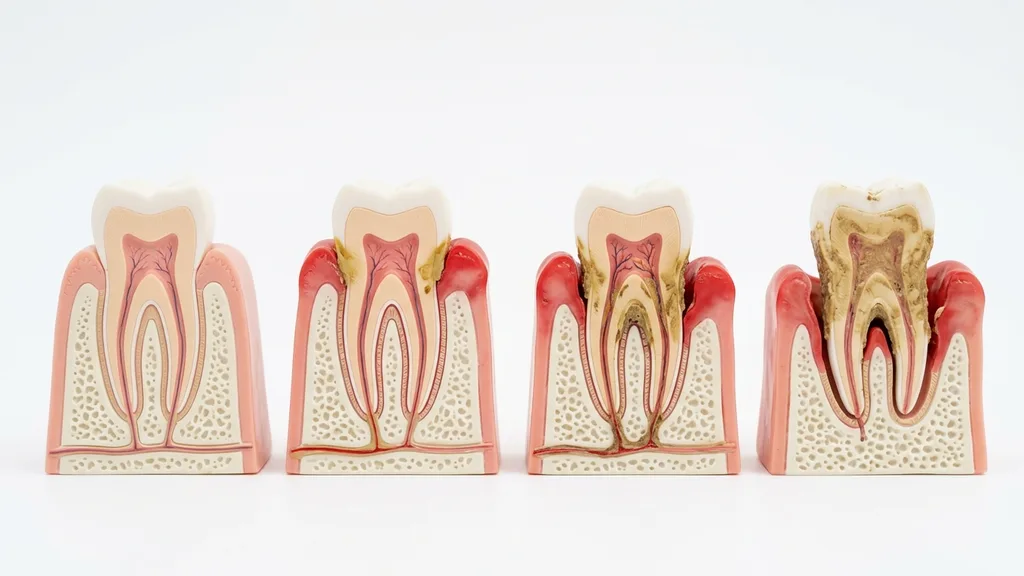
Stages of Periodontitis
Periodontitis is not a uniform disease — it progresses through different degrees of severity, from reversible inflammation to severe bone loss. Understanding the stages helps you assess the urgency of treatment. The decisive rule is: the earlier detected, the better the prognosis.
Stage 0: Gingivitis — The Precursor
Gingivitis is an inflammation of the gingiva that has not yet caused bone or tissue loss. The gums are reddened, swollen and bleed when brushing. Periodontal pocket depths are not increased (≤3 mm). The key point: gingivitis is completely reversible. A professional dental cleaning combined with consistent home oral hygiene is sufficient to fully resolve the inflammation. This stage should be understood as a wake-up call — acting now prevents periodontitis.
Stage I: Mild Periodontitis
In the first stage of periodontitis, the inflammation spreads to the deeper structures. Early bone loss occurs and periodontal pocket depths deepen to 3–4 mm. This stage is often still nearly painless — patients may only notice occasional gum bleeding. X-rays show first signs of bone resorption at the tooth roots. With consistent anti-infective therapy (closed subgingival scaling and root planing), the disease can be very well controlled at this stage and the prognosis is excellent.
Stage II: Moderate Periodontitis
In moderate periodontitis, bone loss has reached a moderate extent. Periodontal pockets deepen to 4–5 mm, the gums recede and tooth necks become visible. Patients now notice more pronounced bad breath, sensitive tooth necks and possibly early tooth loosening. Treatment is more demanding — often several sessions of subgingival scaling are required. At this stage, regular supportive periodontal therapy (SPT) after treatment is particularly important to prevent recurrence.
Stage III/IV: Severe Periodontitis
In the severe stage, bone loss is far advanced. Periodontal pockets of 6 mm and deeper are typical, teeth loosen considerably, tooth migration and bite changes occur. Without treatment, tooth loss is imminent. At this stage, closed therapy alone is often insufficient — surgical interventions (flap surgery) or regenerative procedures may be required. For patients with severe bone loss, we also offer bone regeneration with state-of-the-art biomaterials to restore lost structures and create the foundation for implants.
The most important conclusion: every stage is treatable — but acting early avoids complex and costly interventions. If you recognise any of the described stages in yourself, make an appointment today by calling 089 95760618.
Causes and Risk Factors
The primary cause of periodontitis is the bacterial biofilm (plaque) below the gum line. In deep periodontal pockets, anaerobic (oxygen-averse) bacteria can colonise, producing aggressive enzymes and toxins that trigger an excessive immune response in the body — and it is this immune response that ultimately destroys the bone. Bacterial colonisation alone, however, is not sufficient to trigger severe periodontitis: individual risk factors largely determine who becomes ill and how quickly the disease progresses.
The most important risk factors:
- Smoking — risk factor number one: Smokers have a up to 6-fold increased risk of periodontitis. Nicotine reduces blood flow to the gums, dampens the immune response and masks symptoms such as gum bleeding — which means smokers often notice the disease even later. Smoking cessation is the single most effective measure for improving the periodontitis prognosis.
- Diabetes mellitus: The relationship between diabetes and periodontitis is bidirectional: poorly controlled blood sugar promotes inflammation and worsens periodontitis; at the same time, periodontitis impairs blood sugar control. Diabetics should pay particular attention to their oral health and attend more frequent recall appointments.
- Genetic predisposition: Studies show that genetic factors explain approximately 30% of the variance in periodontitis risk. If close relatives have had periodontitis or have lost teeth, the risk is elevated — regardless of oral hygiene and other factors.
- Stress: Chronic stress increases cortisol levels and acts immunosuppressively. The immune system is less able to combat periodontopathogenic bacteria effectively, and inflammation progresses more rapidly.
- Hormonal changes: Pregnancy, menopause and hormonal contraceptives can make the gums more sensitive. Pregnancy gingivitis affects many women and can develop into periodontitis.
- Medications: Many medications (antihypertensives, antiepileptics, immunosuppressants, antihistamines, antidepressants) cause dry mouth or gingival hyperplasia, which predispose to periodontitis.
- Inadequate oral hygiene: Insufficient tooth brushing and absent interdental cleaning lead to plaque accumulation — the direct cause of gum inflammation and periodontitis.
Systemic associations — why periodontitis affects the whole body:
Periodontitis is not just a "dental problem". Chronic periodontal inflammation releases inflammatory mediators that act systemically. Scientifically established associations include:
- Cardiovascular disease: Periodontitis increases the risk of heart attack and stroke
- Diabetes complications: Deterioration of blood sugar control
- Respiratory diseases: Periodontal bacteria can be aspirated into the lungs
- Pregnancy complications: Increased risk of premature birth and low birth weight
- Rheumatoid arthritis: Bidirectional association with shared inflammatory pathways
These systemic associations underscore why consistent periodontitis treatment protects not only your teeth but your overall health.
Treatment — From Diagnosis to Aftercare
Periodontitis treatment follows a clear, scientifically grounded step-by-step protocol. The goal: halt inflammation, eliminate bacterial load, stabilise the periodontium and prevent recurrence through lifelong aftercare. At our practice in Munich-Oberföhring, we work in accordance with the current guidelines of the German Society of Periodontology (DGParo) and the European Federation of Periodontology (EFP).
-
Periodontal Charting — The Diagnosis
Everything begins with thorough diagnostics. The Periodontal Screening Index (PSI) provides an initial overview. As part of the detailed periodontal chart, we measure probing depths at 6 measurement points per tooth, record bleeding on probing (BOP), tooth mobility grades and furcation involvement. We supplement this with a digital X-ray to assess bone loss. This charting forms the basis for diagnosis, treatment planning and subsequent monitoring.
-
Pre-treatment — Inflammation Reduction and Oral Hygiene Instruction
Prior to the actual periodontitis therapy, we carry out a professional dental cleaning (prophylaxis) and remove supra- and subgingival calculus deposits. Equally important: we instruct you in optimal home oral hygiene — brushing technique, selection of the right interdental brushes and the use of supplementary aids. Optimised oral hygiene is a prerequisite for the success of any periodontitis therapy.
-
Closed Periodontal Therapy (Anti-infective Therapy) — The Core of Treatment
The anti-infective therapy (AIT), also known as subgingival scaling and root planing, is the cornerstone of treatment. Under local anaesthesia, bacterial biofilm, calculus and infected root cementum are removed from the periodontal pockets using ultrasonic instruments and hand instruments (Gracey curettes). Treatment is carried out quadrant by quadrant over several sessions. Smoothing of the root surface makes it more difficult for bacteria to recolonise.
-
Re-evaluation — Assessment of Outcomes after 6–8 Weeks
Approximately 6–8 weeks after the AIT, the re-evaluation takes place: we re-measure all probing depths and document the healing. Bleeding indices and pocket reduction show how successful the therapy was. For most patients, closed therapy is sufficient to stabilise the disease.
-
Surgical Therapy if Required — When Closed Therapy is Insufficient
In the case of persistent pockets exceeding 5–6 mm or unfavourable tooth anatomy, surgical therapy may be necessary. Flap surgery (access flap) provides direct access to deeper root and bone areas. Regenerative procedures such as enamel matrix proteins (Emdogain) or guided tissue regeneration (GTR) with bone substitutes can, in selected cases, partially restore lost bone and periodontal attachment. For further information, visit our periodontology page.
-
Supportive Periodontal Therapy (SPT) — Lifelong Aftercare
SPT is not optional but a necessity: periodontitis is a chronic disease that recurs without regular aftercare. As part of SPT, we carry out an individual prophylaxis and check-up 2–4 times per year — depending on your risk profile and treatment outcome. Statutory health insurance covers SPT for 2 years following systematic periodontitis therapy.
Costs & Insurance Coverage
Since 1 July 2021, the situation for statutory health insurance patients has fundamentally improved: with the new PAR directive, statutory health insurance (GKV) now covers systematic periodontitis therapy as a standard benefit for the first time — a significant advance in the care of periodontitis patients in Germany.
What GKV covers (statutory benefits):
- Periodontal charting (PSI): Screening is covered every 2 years from age 18 as a statutory benefit
- Closed periodontal therapy (AIT): Subgingival scaling and root planing are fully covered by statutory insurance when a documented PSI score of 3 or higher is present
- Supportive periodontal therapy (SPT): Aftercare is covered by GKV for 2 years following completed systematic therapy
- Surgical therapy if required: Also a statutory benefit when medically necessary following re-evaluation
Requirements for GKV coverage: The PAR directive requires a documented PSI code of 3 or higher. The diagnosis must be correctly documented and treatment must follow the prescribed step-by-step protocol. At our practice, we handle all documentation and submission on your behalf.
Co-payments and private services:
- Regenerative procedures (Emdogain, bone substitutes): These high-quality tissue regeneration therapies are billed as private services. Costs depend on the scope of the procedure and are set out in your individual treatment and cost plan.
- Laser treatment: Supplementary laser treatment within the pockets is billed privately
- Extended diagnostics: e.g. cone beam computed tomography (CBCT) or microbiological diagnostics
Private health insurance: Depending on the tariff, private health insurance (PKV) patients may be entitled to up to 100% of treatment costs, including regenerative procedures and laser treatment. We are happy to provide a detailed cost estimate for your insurance.
Financing: For private services, we offer instalment payment and individual financing solutions. Please speak to us — we will find a solution that suits your circumstances together. Call us at 089 95760618 or book a consultation appointment.
Preventing Periodontitis
Periodontitis is in many cases preventable — at least in its severe forms. Gingivitis, the precursor, is completely reversible. Those who act early and practise consistent prevention can prevent gum inflammation from developing into periodontitis. These measures have the greatest effect:
1. Interdental Cleaning — The Absolutely Decisive Factor
A toothbrush alone cleans only approximately 60% of tooth surfaces. The interdental spaces — where periodontitis most frequently begins — remain uncleaned. Interdental brushes are more effective for most patients than dental floss because they remove more plaque and are easier to handle. Use the smallest size that still feels resistance. Once a day in the evening before brushing is sufficient — but daily is essential.
2. Professional Dental Cleaning — Regular and Consistent
Bacterial biofilm that is not removed for a longer period mineralises into calculus — which can no longer be removed at home. Regular professional dental cleaning (prophylaxis) at our practice removes calculus, staining and stubborn deposits in areas that cannot be reached at home. The recommended interval: 1–2 times per year for healthy patients, more frequently for patients with elevated risk or following periodontitis treatment.
3. Smoking Cessation — The Single Greatest Risk Factor
Smoking is the most significant modifiable risk factor for periodontitis. Even after just one year without smoking, the periodontitis prognosis improves considerably. Those who stop smoking reduce their periodontitis risk to the level of non-smokers — an enormous benefit for oral health and general health.
4. Diabetes Management
Patients with diabetes should consistently control their blood sugar — not only for their general health, but also to minimise the risk of periodontitis. The bidirectional association means: better blood sugar control protects the gums, and healthy gums facilitate blood sugar control.
5. Stress Reduction
Chronic stress increases the level of inflammation in the body and weakens the immune system. Stress management techniques — exercise, meditation, adequate sleep — contribute indirectly to oral health.
6. Regular Dental Check-ups
The Periodontal Screening Index (PSI) should be carried out every 2 years — for GKV patients from age 18, this is covered as a statutory benefit. This allows us to detect early signs of periodontitis before bone loss occurs.
The most important message: gingivitis is reversible — act before it becomes periodontitis. If you notice that your gums are bleeding or receding, do not hesitate and book an appointment by calling 089 95760618.

Frequently Asked Questions about Periodontitis
Here you will find answers to the questions our patients ask us most frequently. Further detailed answers can be found in the FAQ section further down on this page.
Is periodontitis curable?
Periodontitis is not "curable" in the classical sense — bone once lost can only be regenerated to a limited extent. However, the disease is very well treatable and controllable. With systematic therapy and consistent aftercare (SPT), the disease can be permanently stabilised. The vast majority of patients keep their teeth for life — if treatment is started in time.
Does periodontitis treatment hurt?
Closed periodontitis therapy (AIT) is performed under local anaesthesia, so you will not feel anything during treatment. In the first few days afterwards, there may be temporary discomfort, gum bleeding and sensitive tooth necks — these typically subside within a few days. We will advise you on appropriate aftercare and pain management.
Does health insurance cover the treatment?
Yes — since the PAR directive of 2021, GKV covers systematic periodontitis therapy as a statutory benefit when a PSI score of 3 or higher is documented. This includes periodontal charting, AIT and SPT for 2 years. Supplementary services such as regenerative procedures or laser treatment are private services.
At what age can you get periodontitis?
In principle, periodontitis can occur at any age — including in young people. However, it most commonly occurs from age 40 onwards: more than 50% of those over 40 are affected. However, there are also aggressive forms that occur in adolescents and young adults. Regular check-ups are therefore important for all age groups.
Do you have further questions? Call us at 089 95760618 or take a look at our comprehensive periodontology page.
Kosten im Überblick
| Leistung | Preisrahmen | Hinweis |
|---|---|---|
| Periodontal charting (PSI) | Covered by insurance | Screening every 2 years from age 18 |
| Closed periodontal therapy (AIT) | Covered by insurance | GKV since 2021 (PAR directive) |
| Supportive periodontal therapy (SPT) | Covered by insurance (2 years) | Aftercare following systematic therapy |
| Regenerative / laser therapy | Private service, depending on scope |
Periodontal charting (PSI)
Covered by insurance
Screening every 2 years from age 18
Closed periodontal therapy (AIT)
Covered by insurance
GKV since 2021 (PAR directive)
Supportive periodontal therapy (SPT)
Covered by insurance (2 years)
Aftercare following systematic therapy
Regenerative / laser therapy
Private service, depending on scope
Private insurance covers up to 100% of treatment costs depending on the tariff, including regenerative procedures and laser treatment.
Instalment payment and individual financing solutions available for private services.
Risiken und Sicherheit
Periodontitis treatment is a proven, safe procedure. Side effects are generally temporary and well manageable.
Postoperative sensitivity and gum bleeding
Common, temporary (a few days)
Resolves spontaneously; chlorhexidine mouth rinse
Exposed tooth necks after swelling subsides
Possible
Aesthetically correctable; desensitisation possible
Recurrence with inadequate aftercare
Preventable
Regular SPT appointments, consistent oral hygiene
Through gentle ultrasonic instruments, minimally invasive techniques and a structured SPT programme, we minimise complications and maximise treatment success.
Qualifikationen und Zertifikate
2012
Licensed dentist (State Examination)
Heinrich-Heine University Düsseldorf
2017
Curriculum in Periodontology
Deutsche Gesellschaft für Parodontologie (DGParo)
2020
Advanced training in regenerative periodontal therapy
DGParo
2017
Member of the German Society of Periodontology (DGParo)
DGParo
Häufige Fragen
Ready to take your first step?
Book an appointment for a personal consultation at our practice in Munich Oberföhring.

